What is a wisdom tooth?
A wisdom tooth, also known as the third molar, is the last tooth in the arch found at the back of the mouth. It generally erupts between the ages of 17 and 25.
You may have 1-4 wisdom teeth or even none!
When must I remove my wisdom teeth?
About 85 per cent of wisdom teeth require removal (according to the American Association of Oral and Maxillofacial Surgeons) because of impaction.
Occasionally, wisdom teeth may also be indicated for removal as part of an orthodontic treatment plan.
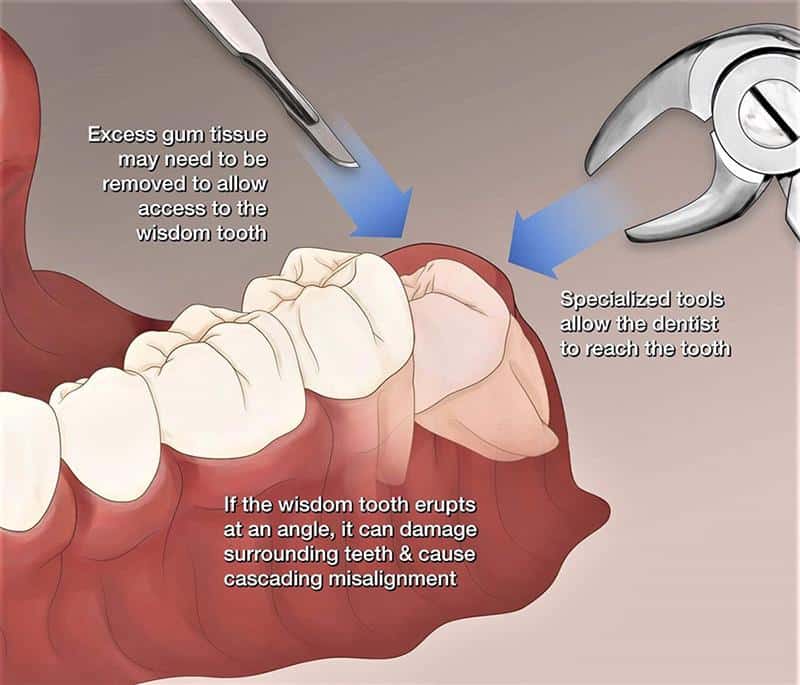
An impacted wisdom tooth occurs when the tooth does not completely erupt into the mouth, leaving it partially-covered by gum tissue. A pocket tends to form in between the loose gum and the tooth. This pocket can trap food and bacteria if it is not cleaned out regularly and this can lead to an infection of the gum that is partially covering the wisdom tooth (pericoronitis). The adjacent tooth may also start to decay because of the food accumulation caused by the impacted wisdom tooth. Pressure from the impacted tooth on the adjacent tooth’s roots may cause resorption (dissolving of the root). For these reasons, it maybe recommended that you remove your impacted wisdom teeth, even if they are not causing discomfort.
We may advise you to remove a non-impacted wisdom tooth if it is severely decayed, causing repeated frictional ulcers in the cheek or if it has drifted out of position to impinge on the gum of the opposing arch.
An infected and impacted wisdom tooth may cause the following symptoms:
- Pain, swollen/tender/bleeding gums with pus discharge
- Swelling in the jaw area
- Bad breath
- Unpleasant taste in the mouth near the affected teeth
- Headache/jaw ache
- Difficulty opening the mouth
- Difficulty swallowing
- Swollen lymph nodes along the jawline and neck
- Fever
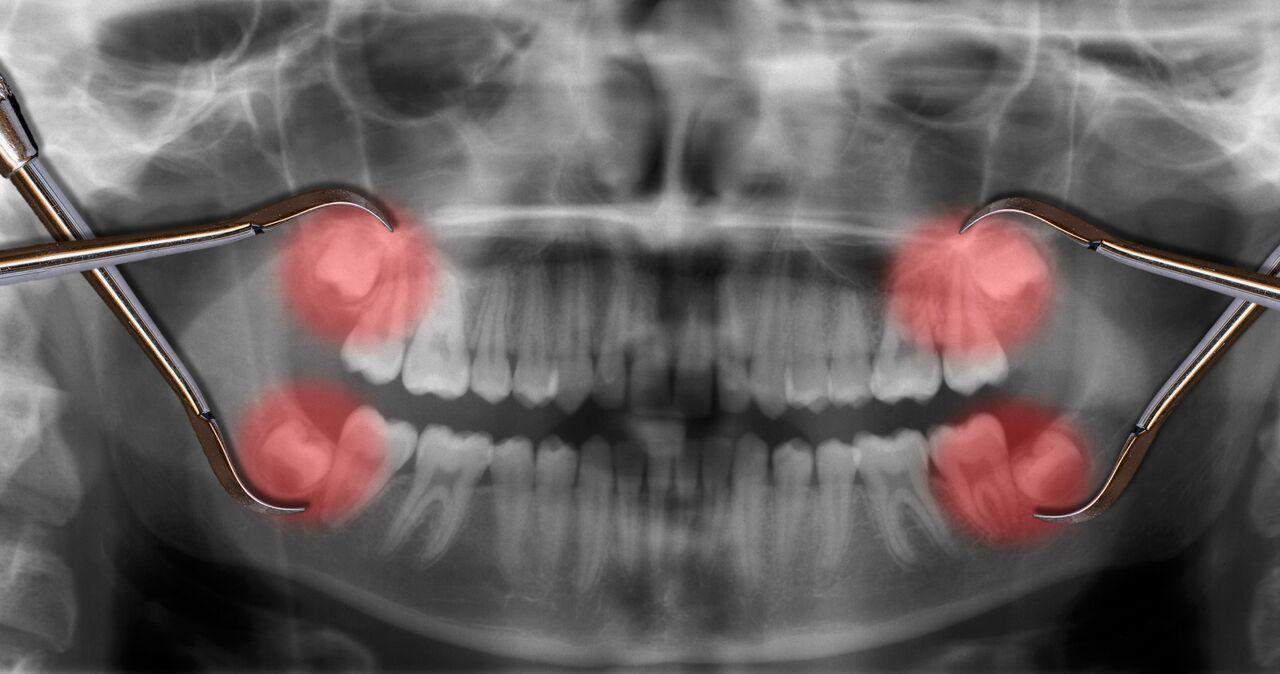
Wisdom Tooth Surgery at Elite Dental
Step 1: Consultation
Your wisdom teeth will be assessed as part of your new patient examination or as part of active maintenance visits.
Radiographic assessment is a routine part of the pre-surgical planning. We may order a 3D CBCT Scan that will provide more information about your wisdom tooth and its relationship with surrounding teeth and other structures (nerves, sinuses) within the bone.
Step 2: Pre-surgical preparation
A few days before, a thorough scaling and polishing is done. An oral probiotic is also given to boost the numbers of beneficial bacteria in the saliva so that healing is smooth.
Step 3: Removing the wisdom tooth
The wisdom tooth is always removed under a local anaesthetic. You may also choose to be sedated for the entire procedure to ensure an anxiety free procedure.
Your tooth may need to be sectioned to allow for a gentle removal with minimal trauma to the surrounding tissues. Stitches will then be placed in the gums afterward. These will be removed after a few days when healing is complete. A gauze pack will be placed over the wound to encourage blood clotting and to stop bleeding.
It is important to note that if you are Singaporean or a Singapore PR, we may help you make a claim against your Medisave account to pay for your wisdom tooth surgery either partially or in full.
General advice for recovery from Wisdom Tooth Surgery
- Have plenty of cold food (ice cream, milkshakes) and iced drinks on the day of surgery. Some patients like to hold ice cubes in the mouth to minimise pain and swelling.
- Have soft foods after surgery, for example, congee, yoghurt, soft boiled eggs
- Apply lip balm to keep your lips moist
- Rinse gently with salt water after meals. Hold the salt water in your mouth for about 5 minutes before spitting out.
- Start all rinses 24 hours after surgery, not sooner.
- DO NOT SMOKE!! This will interfere with proper wound healing.
- Avoid vigorous exercise.
- Remember to take your medication – set a timed alarm on your phone if necessary.
[su_button url="other_services" style="default" background="#003853;" size="6" wide="yes" center="yes" radius="0"]TO SERVICES[/su_button]





